How Do IUDs Work?
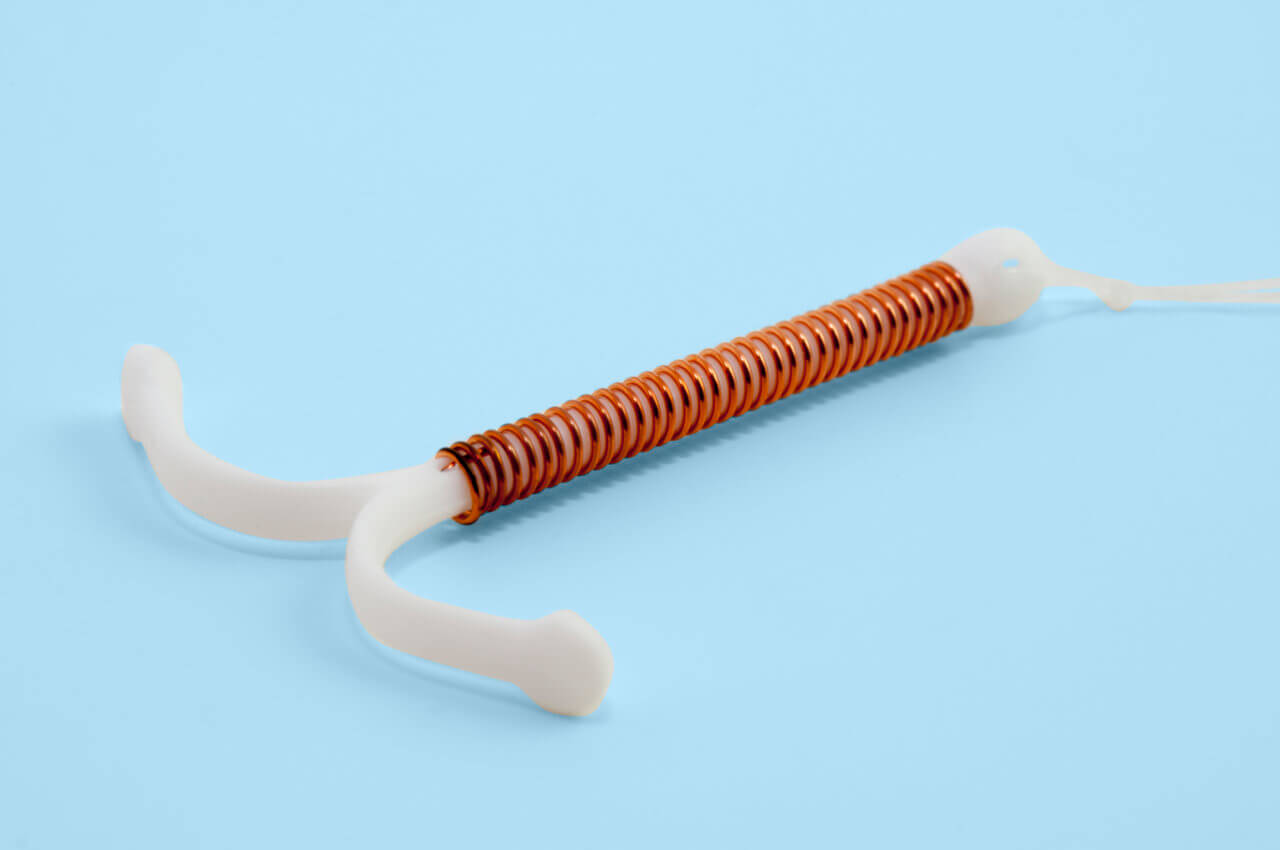
An IUD (intrauterine device) is a type of birth control. It’s a “T” shaped device slightly larger than a quarter that a healthcare provider puts into your uterus to prevent sperm from fertilizing eggs.
Types of IUDs
There are five types of IUDs available in the U.S. Four of the five (Liletta, Kyleena, Mirena, and Skyla) prevent pregnancies by releasing small amounts of a hormone called progestin into the uterus. This is the same hormone found in many types of birth control pills. These IUDs may make your periods lighter, which is an added benefit if you have heavy periods.
The fifth type of IUD, ParaGard, is a hormone-free version that releases copper ions into the uterus, creating an environment that stops sperm activity. Copper IUDs may make your period heavier, but they last longer than hormonal IUDs. If you choose to use an IUD, you should consider those factors among others.
How Effective Are IUDs?
IUDs are highly effective. When you use one correctly, the chance of getting pregnant is less than 1%.
The copper IUD is also extremely effective as a form of emergency contraception. When inserted within 120 hours (five days) after unprotected sex, it is 99.9% effective in preventing pregnancy.
Who Can Use an IUD?
Most healthy women can use an IUD. They’re best for those with one partner a low risk of contracting a sexually transmitted disease (STD).
There are a few cautions about IUDs in general, including that you shouldn’t use one if you:
- Are pregnant
- Have cervical or uterine cancer
- Have vaginal bleeding without a known cause
- Have an STD or recently had a pelvic infection
It’s safe to use a hormonal IUD unless you have breast cancer or a high risk of developing it or you have liver disease.
Regarding copper IUDs, you can’t use one if you’re allergic to copper or have Wilson’s disease, which makes your body retain excessive copper.
Also, it’s difficult for a healthcare professional to place an IUD properly for some women due to the size or shape of their uterus.
IUD Pros and Cons
As with any form of birth control, IUDs have pros and cons.
IUD Pros
- They’re highly effective.
- They’re convenient.
- The hormonal versions may lighten your periods.
- They’re removable if you decide you want to get pregnant.
- They’re cost-effective in the long term.
- They last from 3 to 12 years, depending on the manufacturer.
- Copper IUDs begin working immediately after insertion, and hormonal versions start working within 7 days.
IUD cons
- They don’t prevent STDs.
- Insertion ranges from uncomfortable to painful.
- Their upfront cost can be high if you don’t have health insurance.
- A copper IUD can make your periods heavier.
- There are risks of complications like harmless ovarian cysts, pelvic inflammatory disease, or a uterus perforation during insertion.
Other Important Considerations for Using an IUD
There are possible side effects of having an IUD inserted. They include feeling dizzy or lightheaded for a few minutes after insertion and experiencing cramping and bleeding for a few days. There is also the risk of becoming pregnant. That risk is very low, but if you conceive, your IUD puts you at a higher risk of miscarriage or ectopic pregnancy.
Your partner shouldn’t feel the IUD during sex. If they do, they will only sense the IUD strings and shouldn’t experience discomfort.
It’s rare, but an IUD can come part way or all the way out. That’s more common if you’re under 20 years of age, have uterine fibroids, haven’t had children, or have the device inserted soon after having a baby.
It’s important to note that IUDs don’t cause abortions. That’s a common misconception. They only prevent pregnancies from occurring.
Having an IUD placed takes just a few minutes at your doctor’s office. And you can have a new IUD inserted in the same appointment when you have an old one removed.
Learn About IUDs From Your Baptist Health Physician
If you have questions about IUDs or other forms of birth control, we’re happy to answer them! You can talk with your primary care physician or one of our women’s services specialists.
Next Steps and Useful Resources
5 Things to Know Before Getting a Vasectomy
Treat Endometriosis Using Birth Control
What Is an Ectopic Pregnancy?



